The Friction Issue: A V.supple Skin Edit for the Parts of You No One Talks About
From bra bands to bike seats and radiotherapy gowns - how everyday friction rewires sensitive skin, and what science led care can actually undo.
When friction becomes a diagnosis
For many women, there is a moment when ordinary fabrics and seams no longer feel ordinary.
The bra band that digs in by 3 pm. The waistband that leaves a burning mark. The bike seat, saddle, or desk chair that suddenly feels unforgiving. The vulva that stings after a day in basic underwear, or the radiotherapy field where even soft cotton rubs like sandpaper.
We are taught to call it “dryness” or “sensitivity”. In reality, what is happening in the skin and mucosa is more complex. Hormonal change, weight shifts, cancer treatments, surgery and ageing collagen all turn everyday friction into a genuine clinical stressor.
In this V.supple Skin Edit, we map the new “friction zones”, look at what is happening inside the tissue, and outline a science based friction care ritual - including where non hormonal products such as V.supple® Balm and DermaVeil+ (Coming Soon) may sit within medical care.
The Friction Map - 9 zones that change after 40
Friction affects more than one place. Once oestrogen declines or major treatments occur, the body becomes a map of new hotspots.
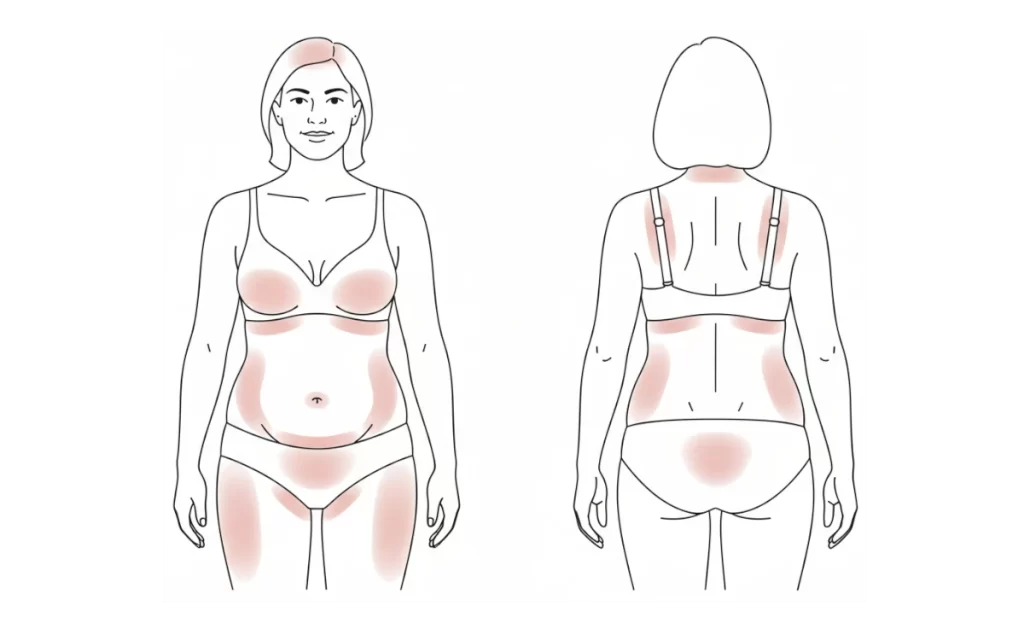
1. Scalp and hairline
Headbands, wigs, helmets and tight ponytails can irritate thinner, drier skin, especially after chemotherapy or endocrine therapy.
2. Under bra bands and under bust
Loss of dermal thickness and elasticity means the same bra band now delivers a higher “dose” of pressure and shear to the skin.
3. Nipples and areolae
Post surgery, post radiotherapy or with hormonal treatments, this area can become exquisitely sensitive, with friction from bras or seams triggering burning or stinging.
4. Under belly and waistbands
Weight redistribution and abdominal folds create moist, warm friction zones that are prone to chafing, maceration and secondary infection.
5. Groin folds and inner thighs
Walking, sport, and simply existing in certain fabrics can cause repeated rubbing, especially when natural lubrication and barrier lipids are reduced.
6. Vulva and perineum
With genitourinary syndrome of menopause (GUSM), cancer treatments or chronic dermatological conditions, friction from everyday underwear, pads, sex, or even washing can feel dramatically different.
7. Perianal area
Radiotherapy, altered bowel habits, loose stools, and frequent wiping can make this tissue thin, friable and friction sensitive.
8. Necklines and shoulder straps
Bra straps, camisoles and mask ties can rub where the skin has been irradiated or has lost elasticity.
9. Hands and high contact areas
Constant washing, sanitiser and manual tasks strip lipids and disrupt the barrier, making any tool, glove or surface feel harsher than it should.
You may recognise yourself in one or many of these zones. The common thread is not “being fussy”. It is tissue that now behaves differently under mechanical load.
Inside the tissue - what friction does to collagen, nerves and the microbiome
Friction on healthy, oestrogen replete skin is not the same as friction on thinned, irradiated or inflamed tissue.
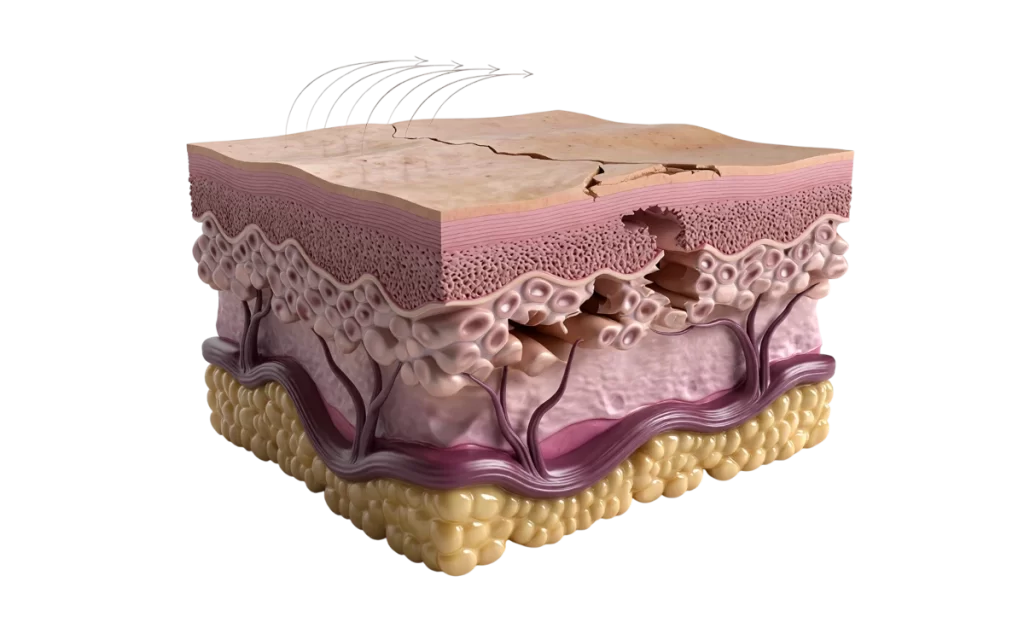
Key changes include:
- Collagen and elastin loss
With age and low oestrogen, dermal collagen decreases and elastic fibres are altered. The skin becomes less able to buffer pressure and shear, so the same seam or seat now transmits more force to nerves and microvessels. - Thinner epithelium and mucosa
In the vulva, vagina and perianal area, the epithelial layer can become thinner and less glycogen rich. This makes micro tears and fissures more likely with intercourse, clothing and wiping. - Reduced lipids and natural moisturising factors
Decreased sebum and altered lipid composition mean less “built in lubrication”. Without that thin lipid film, surfaces catch instead of glide. - Nerve hypersensitivity
After surgery, radiotherapy or chronic inflammation, nerve endings may be closer to the surface or sensitised. Low level friction that used to be ignored is now interpreted as burning, stinging or electric pain. - Microbiome disruption
Changes in pH, moisture and local immunity alter the bacterial and fungal communities, particularly in occluded folds and intimate areas. Friction on already inflamed or overgrown skin becomes a multiplier for symptoms.
When a woman says “my skin just cannot cope any more”, it is usually this mix of structural, biochemical and neurological change underneath a very simple action - fabric against skin.
Your 3 minute Friction Audit
This simple self check can help you understand your own friction map and gives language to take into an appointment.

Over the past 7 days:
- By the end of the day, which of these felt sore, rubbed or burning?
- Bra band
- Under bust fold
- Waistband or under belly fold
- Groin folds or inner thighs
- Vulva or perineum
- Perianal area
- Radiotherapy field or surgical scars
- Have you changed fabrics, cuts or sizes recently simply to “get through the day” with less rubbing or stinging?
- Do you avoid specific activities because of friction discomfort?
- Long walks
- Cycling or horse riding
- Sitting for long periods
- Sex
- Wearing bras or fitted clothes
- Do you notice micro cuts, fissures, or bleeding after friction (for example after intercourse, bowel movements or exercise)?
- On a scale of 1 to 5, how often does friction make you consciously aware of a body area:
- 1 = almost never
- 3 = a few times a week
- 5 = most days or most activities
A high “friction score” does not mean you are imagining things. It suggests that your tissue may need both mechanical change and targeted barrier support, and sometimes medical assessment.
The science backed Friction Edit - three precise moves
1. Reduce avoidable friction
Before adding products, reduce the mechanical load:
- Refit bras and underwear to ensure correct band and cup size.
- Prefer soft, low seam garments and avoid abrasive lace directly on stressed areas.
- For sport, consider chamois creams, saddle re fitting, or specialist shorts guided by a physiotherapist or sports fitter.
- Review pads, liners and incontinence products with a continence nurse or pelvic health specialist where relevant.
The goal is not to “baby” the skin, but to remove unnecessary friction so the tissue can respond to treatment rather than constant micro injury.
2. Rebuild the barrier and hydration architecture
Here, formulation science matters more than marketing language.
- Hydration with intelligent hyaluronic delivery
Microsphere hyaluronic technology, as used in V.supple® formulations, employs tiny cross linked spheres of hyaluronic acid. These sit within the superficial layers and gradually release moisture, acting as micro reservoirs. This supports water binding and viscoelasticity over time rather than a short lived surface film. - Emollients and lipids to reduce shear
Ingredients such as caprylic/capric triglycerides and cold pressed avocado oil help replenish lipids, soften the stratum corneum and create a more glide friendly interface between fabric and skin. - Barrier support for compromised or post treatment skin
In areas affected by radiotherapy or procedures, a structured barrier product such as DermaVeil+ with multi type hyaluronic acid and ceramides can help restore barrier integrity, calm reactivity and reduce the impact of unavoidable friction from clothing or movement.
Used one to three times daily, particularly after showering and before known friction exposures, this approach can convert a raw, catch prone surface into one that tolerates the day with less trauma.
3. Escalate when friction is a red flag
There are clear points where friction symptoms should prompt medical review rather than endless self management:
- Persistent fissures, cracks or ulcers
- Bleeding, especially in radiotherapy fields or intimate areas
- White, shiny, thickened or scar like patches on the vulva or perineum
- Sudden change in symptoms without a clear trigger
- Pain that feels disproportionate to visible changes
At this point, assessment by a vulval dermatologist, sexual health physician, oncologist or gynaecologist is crucial. Non hormonal products such as V.supple® Balm, pessary preparations, or barrier gels may be part of the plan, but they should sit alongside diagnosis, not instead of it.
Micro stories - when we treated friction, not just “dryness”

These anonymised examples are typical of what clinicians hear:
- The breast cancer survivor and the seatbelt
After radiotherapy, a woman found every car journey unbearable. By addressing fabric choice, adding a carefully positioned pad, and introducing a structured post radiotherapy barrier gel, the same seatbelt became tolerable for daily life. - The cyclist in perimenopause
A keen rider began avoiding longer rides because her vulva and inner thighs felt “sandpapered” for days afterwards. Saddle re fitting, padded shorts, and a non hormonal vulval care ritual using a microsphere HA cream before and after rides allowed her to keep her sport rather than abandon it. - The desk based professional
Sitting all day in synthetic underwear and tight trousers left her vulva sore most evenings. A combination of breathable fabrics, cut changes and regular application of a non hormonal vulval balm converted an invisible daily burden into something manageable.
In every case, the turning point was when friction was recognised as a mechanical, biological problem - not “just getting older”.
Bring your Friction Audit to your next appointment
Friction is not a vanity issue. It is a daily, mechanical stress signal from tissues that have changed under the influence of hormones, treatments and time.
If this Skin Edit resonates with you:
- Complete the Friction Audit and note which zones trouble you most.
- Bring your notes to your next appointment with your GP, oncologist, gynaecologist or pelvic health specialist.
- Ask specifically about barrier repair, fabric and garment strategies, and whether a non hormonal intimate care product could have a role in your plan.
V.supple® has been developed within a medical context to support hydration, barrier integrity and comfort in sensitive and intimate skin. It is not a substitute for diagnosis or prescribed treatment. It can, however, be one of the tools that help you live more comfortably in your own skin when friction has quietly become part of your story.

